More Australians with type 2 diabetes should gain access to potentially lifesaving medications, a new analysis has found.
UNSW medical researchers say more Australians with type 2 diabetes need to be offered add-on medications that would better protect them from heart and kidney disease – which are among the major causes of death for people with diabetes.
About one in three people with type 2 diabetes are receiving early treatment with additional medicines that protect their heart and kidneys, new research led by UNSW Sydney shows.
The study, published in The British Journal of Clinical Pharmacology,, opens in a new window analysed dispensing records of a 10% random sample of adults on the Pharmaceutical Benefits Scheme (PBS). It found almost 39,000 people aged 40 and over started on metformin – the first-line treatment for type 2 diabetes – between 2018 and 2020. Only about a third received any add-on therapy within two years of starting their treatment.
“More than one million Australians are living with type 2 diabetes, but it is heart and kidney disease that are major causes of death and poor quality of life for these people,” said lead study author Dr Tamara Milder, an endocrinologist with UNSW’s School of Population Health.
“Fortunately, there are diabetes medicines available that can also protect their hearts and kidneys, and potentially save lives, but many people are missing out.”
It can take time for clinicians to adopt newer medications, as they may be wary of potential side effects and comfortable with medications that they have known for longer time periods, the study notes.
Limited PBS access to these medications – restricted to those with high blood sugar or for whom other subsidised medication had failed – had potentially limited prescribing practices, the researchers added. The COVID-19 pandemic and international shortages of some medications since 2022 may also have had some impact.
Media enquiries
For enquiries about this story and interview requests, please contact Kate Burke, News & Content Coordinator, UNSW Medicine & Health.
Tel: +61 2 9348 2538, opens in a new window
Email: kate.burke@unsw.edu.au

Rapid changes made to diabetes management guidelines
Considerable changes have been made to national and international type 2 diabetes management guidelines in recent years, due to the advent of new tablets and injectable medicines, like Ozempic, Dr Milder said.
“There has been a major shift in recent years in how we treat diabetes,” Dr Milder said. “It used to just be about managing people’s sugars, but we know that heart and kidney disease are major drivers of death and poor quality of life for people with diabetes, and we have these two major drug classes that can help protect people with type 2 diabetes.”
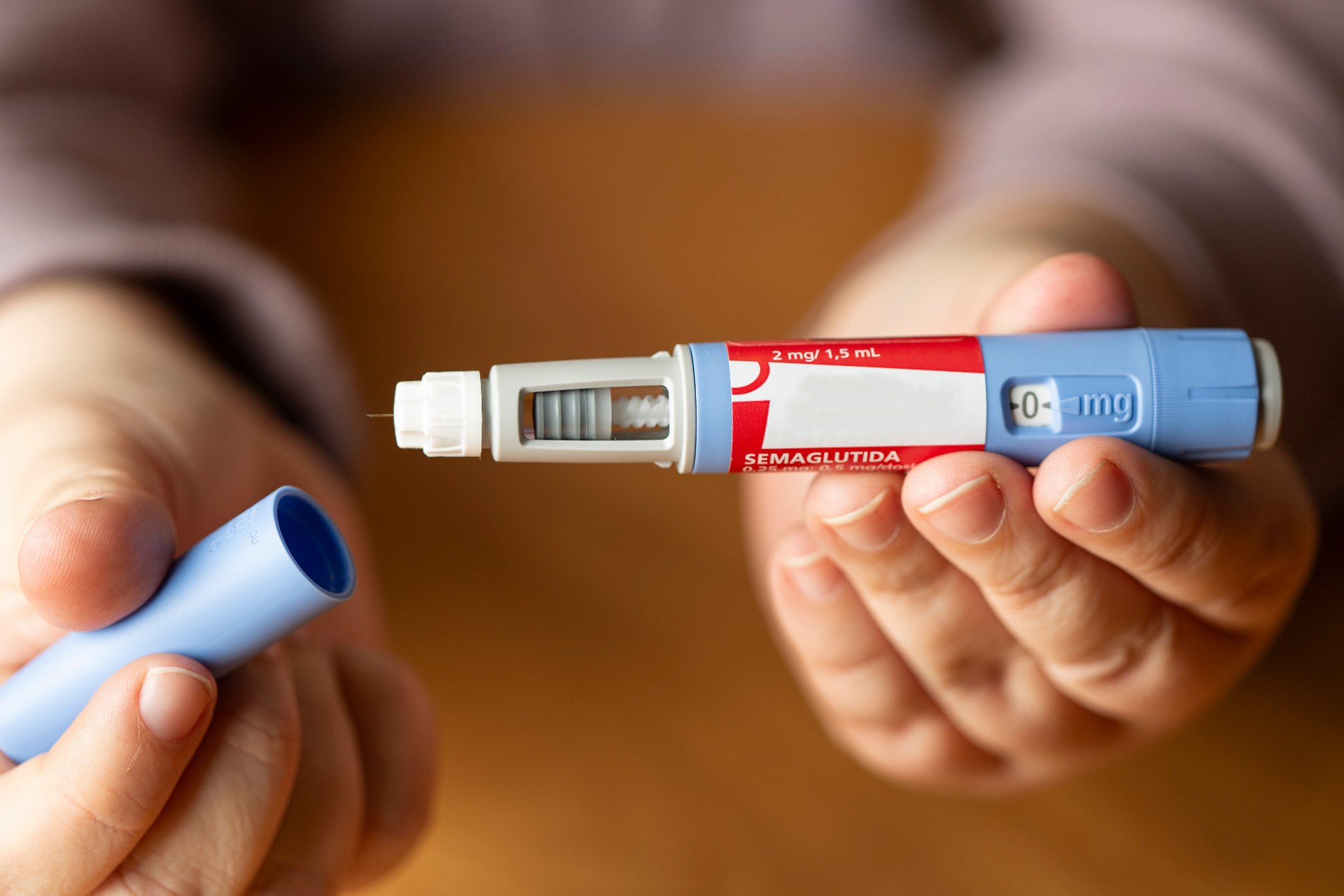
These drug classes, known as SGLT2i (sodium-glucose co-transporter 2 inhibitors) and GLP-1 RA (glucagon-like peptide-1 receptor agonists), help manage and improve blood sugar, but also have additional benefits like weight loss, lowering blood pressure and reducing the risk of kidney and cardiovascular events. Semaglutide, best known by brand name Ozempic, is a GLP-1 RA.
Their benefits were first highlighted in the Australian Diabetes Society’s Type 2 Diabetes Management Algorithm in 2020, before being recommended in 2022 for dual therapy use for adults with type 2 diabetes and cardiovascular disease, multiple cardiovascular risk factors and/or kidney disease.
While it is not known how many people in the sample group would fall into this cohort – or meet existing PBS criteria – people with diabetes are generally at high risk of cardiovascular events, heart and kidney failure, Dr Milder said.
“We have these medications with heart and kidney benefits that we can see are not being heavily used in early treatment, that there are a lot of people who are not having add-on therapy,” Dr Milder said.
While the overall use of add-on therapy remained low, SGLT2i and GLP-1 RA were increasingly used as the first add-on therapy over the analysed period, respectively rising from 28.8% to 35%, and from 3% to 9.6%. They were among six anti-hyperglycaemic medicine classes which the researchers focused on.
Of those people who were given add-on therapy, one third started it on the same day as they began metformin. The remainder waited a median of about eight months before they started on any additional medicine.
Senior report author Dr Michael Falster, also from UNSW’s School of Population Health, said the medications were being increasingly used in people with established cardiovascular disease but were generally being underutilised across the board.
“It's challenging, we have new medicines with fantastic capabilities in helping prevent progression for serious health outcomes, but a slow uptake,” Dr Falster said.
Greater action at a policy level to increase prescribers’ knowledge and confidence to use these medicines was needed, as was more research to better understand gaps in eligible people using these medicines.
The researchers also acknowledged the government was regularly reviewing whether it was cost-effective to expand subsidised prescriptions of these medicines, and noted there were also issues of medication shortages.
“We must ensure there's equitable access to these medicines for the people for whom there's the greatest therapeutic benefit,” Dr Falster said.
Dr Milder added: “We must prioritise early access to these medicines for Australians with type 2 diabetes. By doing so, we can better protect their hearts and kidneys, improving both quality of life and overall health, and saving lives.”